The Problem
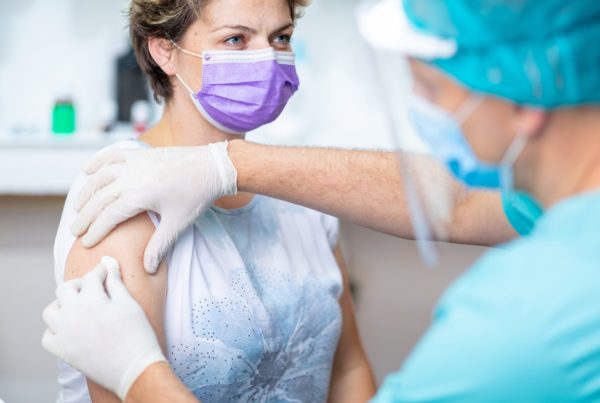
There’s no question that virtual healthcare is on the rise. It’s seen as the wave of the future, a way to make our health care system more efficient and convenient. There are now many providers of this service in Canada.
Virtual care allows you to “see” a doctor in minutes over your mobile phone or on your desktop computer. Typically, the service functions essentially as a virtual walk-in clinic. You won’t see your regular family doctor. It’s more like an “Uber”-ization of health care, as you’ll be connected with any doctor or nurse practitioner employed by the service provider who happens to be available at the time that you request the virtual visit. Some services do allow you to request the same practitioner, but not all do.
Our modern lives are busy. Access to health care, quite frankly, can be difficult and time consuming. Who wants to take the entire afternoon off work for a doctor’s appointment, just to check blood pressure and renew a prescription? Many people with high blood pressure can monitor themselves with reliable home devices. You may not feel you need a doctor to physically take the reading; you just want medical advice as to what to do about it. As another example, who wants to visit a crowded emergency room at two in the morning for a urinary tract infection, when you already know exactly what it is because you’ve had it before?
Virtual care solves a lot of issues like these. It allows you to see a doctor quickly and conveniently. This can be good for patients, doctors, employers and the health care system in general.
The Importance of Continuity of Care
Not all medical problems are appropriate for virtual care, however. Obviously, if you have a symptom like abdominal pain or shortness of breath, a doctor has to see you physically in order to provide a proper assessment.
For other medical problems, we need to remember the importance of continuity of care in the practice of medicine before we decide if virtual care is the best way to address our particular problem. The American Academy of Family Physicians has issued this statement about continuity of care: “Continuity of care is rooted in a long-term patient-physician partnership in which the physician knows the patient’s history from experience and can integrate new information and decisions from a whole-person perspective efficiently without extensive investigation or record review.”
Many medical problems, particularly complex ones that cannot be solved in a single visit, are not best served by seeing a virtual provider. Virtual care, if it’s going to be effective, should not fragment someone’s care. It should not interfere with getting to the best solution to your problem.
As I often tell my patients, when there are too many cooks stirring the pot, problems develop. I see this constantly in the emergency department (ED) where I practice. Patients come in with all sorts of complaints that have been going on for weeks or months. They aren’t experiencing an emergency when I see them and they don’t require hospital admission, but something clearly is not right. I’m compelled to discharge them home to follow up with a health care provider who can arrive at a proper diagnosis. On further inquiry, however, it becomes apparent that they are currently seeing many different doctors in a wide array of settings, trying to get answers for their complaints.
Access issues in our health system often propel patients to seek care in this manner. Many of these patients actually have their own family doctors, but they find it challenging or awkward to get in to see them, so they turn to walk-in clinics instead. When their symptoms come to a head, they use the ED. They end up being told all sorts of different things by the many doctors they interact with, and they become confused and anxious. What one doctor says, the next doctor disagrees with, and off they go in a different direction. They’ve had multiple investigations ordered by the various practitioners they’ve seen. At this point, it’s difficult to decipher what is actually going on.
I tell these patients that it’s extremely important to stick with one doctor. See that doctor regularly, so he or she has the opportunity to understand you and your symptoms over time. The doctor can take a step-by-step approach to the investigation of your problem, trying different treatment approaches, from a lifestyle or a pharmaceutical approach. If tests come back negative, or treatment has no impact on your symptoms, then it is imperative that you circle back to that same doctor to decide on the next approach.
Seeing a virtual care provider is the same as seeing a provider in a walk-in clinic. It’s convenient and helpful if it is a simple medical problem that requires little to no follow-up or requires no long-term management. But for any complex medical problem, it really is best to ensure that you have continuity of care with a single practitioner. That is always the best way to manage one’s health in the long term.
Save the Apps for Uncomplicated Cases
Virtual care is very useful for simple problems that do not require follow-up or ongoing care, such a mild rash, a sinus infection or diarrhea. This “wave of the future” truly can help the health care system by skimming off the medical problems that don’t have much complexity around them, and dealing with them more efficiently.
These problems, however, are not the ones that clog up our system. And the more complex the symptoms become, the less helpful virtual care will be. For instance, titrating medications for blood pressure management or blood sugar control are not best accomplished by involving a different physician each time who has his or her own opinion on how best to adjust the medication dosages. Same goes for someone with recurrent urinary tract infections. You need to have urine cultures done and appropriate follow-up to ensure that the infection has cleared. If it’s not clearing, then an astute clinician will take the next step, sending you for further investigations and a consultation with a urologist.
What if virtual medicine could help us to deliver complex, chronic care more efficiently? This is the most exciting potential for this technology. What if you could see your own doctor virtually when you want? For instance, you might see your regular family doctor physically in the office when you need to but then interact with him using a virtual care app when that’s more convenient and is a medically appropriate option.
This would truly be the best of both worlds, overcoming the continuity-of-care problem inherent in most virtual medicine models.
The challenge in Canada is getting this service covered by our provincial health plans. Governments are likely concerned that allowing medical services to be delivered virtually will increase utilization – and cost. I expect they are approaching this cautiously.
Until then, we are left with virtual care for simple medical problems that require little to no follow-up. And for those problems, it is very helpful and convenient.
For more valuable health information, visit our Ask the Expert section.